What Are the Biggest Mistakes Founders Make When Building EMR?
Last updated:9 April 2026

Sometimes, custom EMR projects can become expensive, slow, and difficult to adopt, even when the goal is clear from the start. Scope gaps and late security decisions often create bigger problems than missing features. But we know how to fix it.
In our new article, we break down the decisions that cause the most damage in custom EMR development. We cover practical pitfalls in custom EMR development: where teams lose time, where usability starts to break down, how security and compliance gaps create risk, and what helps prevent these issues before they affect delivery and adoption.
Key takeaways
- Most mistakes in EMR development begin before development moves too far, usually during discovery, scope definition, and workflow planning.
- When the system does not match how clinicians and staff actually work, adoption drops and workarounds appear quickly.
- A steep learning curve is a major contributor, and with a new system, this is one of the most common pitfalls teams underestimate.
- Early decisions about architecture and integrations shape how easily the EMR can scale, connect to other systems, and adapt over time.
- This is also where data loss and issues with proper data mapping tend to surface if rushed.
- Security and compliance need to be part of product design from the start. Adding new technology or new features after the core architecture is set reopens settled decisions, disrupting what should be a streamlined process.
- A strong custom EMR reduces the risk of HIPAA violations and supports daily clinical work in a way that feels clear, reliable, and practical for end users.
What Is Custom EMR System Development?
Custom EMR system development is the process of designing and building an electronic medical record system around the needs of a specific healthcare organization. Instead of asking teams to adjust their processes to match a prebuilt platform, this approach starts with the way clinicians, administrators, and support staff already work.
Some healthcare teams also use platforms like Medplum as a starting point for FHIR-based infrastructure, patient data workflows, and integrations, then extend that foundation with custom features tailored to their operations.
Key aspects of custom EMR system development
- Alignment with clinical and operational workflows. The system supports real-world processes across roles and specialties. This may include tailored documentation, scheduling logic, role-based access, and internal coordination flows.
- Scope beyond product development. Custom EMR projects include decisions about system architecture, reliability, and long-term support. They are not limited to features or interface design.
- Security and data protection. Implementation of encryption, audit logs, and access controls to ensure patient data is protected and traceable.
- Compliance with healthcare regulations. The system is designed to meet requirements related to data storage, access, and disclosure based on applicable regulations.
- Interoperability with external systems. Integration with billing platforms, laboratories, pharmacies, patient portals, and other healthcare systems using standards such as HL7 or FHIR.
- Control over system behavior and evolution. Custom development allows organizations to define how the system works, how data flows between systems, and how the product adapts over time. This helps address gaps often found in off-the-shelf solutions.
- Focus on internal care delivery workflows. Unlike EHR software development, which often supports broader data exchange across organizations, custom EMR systems are typically centered on managing records and workflows within a specific provider environment.
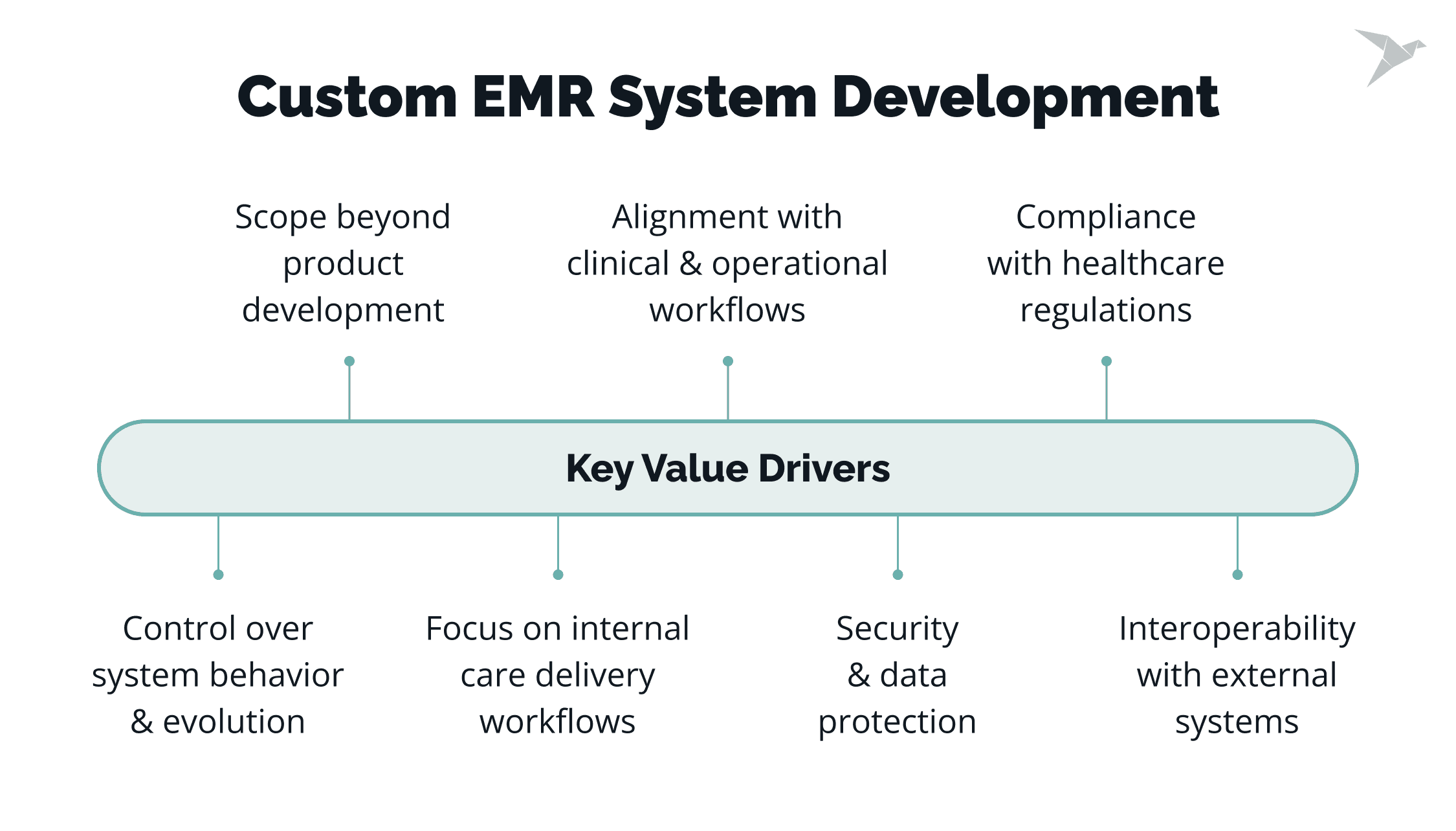
A custom EMR is designed to match how a specific healthcare organization operates, rather than forcing teams to adapt to a predefined system.
What Are the Biggest Mistakes in Custom EMR System Development?
The biggest mistakes in custom EMR development usually start long before launch. Here are the most common issues we see in practice.

Poor discovery and unclear project scope
One of the most common mistakes in EMR building is starting development without a clear definition of what the system needs to support. Clinical workflows, user roles, integration needs, and technical constraints may be only partially documented or understood differently across teams.
This creates gaps between expectations and delivery. New requirements appear mid-project, priorities shift, and scope expands without enough control. It often results in rework, delays, and functionality that doesn’t fully match real operational needs.
Ignoring real clinical workflows and user needs
A custom EMR may still fail if it does not reflect how care teams actually work. When the system is based on assumptions instead of real workflows, users face extra steps, repeated data entry, and navigation that does not match the flow of care.
This slows down routine work and creates friction in daily use. Over time, it also reduces trust in the product and makes adoption harder.
Weak UX and overloaded interfaces
Another major pitfall in EMR building is treating UX as a secondary concern. EMR systems are complex by nature, but that does not mean interfaces should be cluttered or hard to scan.
When screens are overloaded, and workflows feel inconsistent, users spend more time searching, clicking, and correcting mistakes. Even strong functionality loses value when the system is difficult to use.
Bad architecture decisions that limit scaling
Some custom EMR platforms work in the first release but become difficult to extend later. This often happens when early architectural decisions prioritize speed over flexibility.
Tightly connected components, rigid data models, and limited modularity make future changes slower and more expensive. As the system grows, these issues turn into long-term delivery and maintenance problems.
Underestimating the integration and EHR system's interoperability complexity
Custom EMRs rarely operate on their own. They usually need to connect with labs, billing tools, patient portals, pharmacies, and other clinical systems.
In practice, healthcare integrations are complex. Different systems handle data differently, and interoperability standards still require careful implementation. When this work is underestimated, teams end up with fragmented data flows and manual workarounds.
For teams building around modern interoperability standards, platforms such as Medplum can simplify part of this work. They provide a FHIR-native base for data exchange and workflow orchestration. Pay attention that they do not remove the need for careful integration planning, mapping, and validation.
No realistic rollout, validation, or feedback process in EHR implementation
A custom EMR succeeds when users can rely on it in real clinical settings. A common mistake is launching too broadly, with too little validation and no structured feedback loop.
That increases the risk of disruption during live use. Problems appear too late, confidence drops quickly, and adoption becomes harder to stabilize.
Insufficient training and go-live support
Even a well-designed system can struggle if users are not prepared to work with it. Training is often treated as a final step instead of part of successful implementation.
This leads to slower adoption, inconsistent feature use, and more documentation errors during go-live. In practice, weak training and support can undermine the value of the whole system.
These pitfalls in EMR building have the biggest impact because they affect usability, delivery, interoperability, and long-term adoption at the same time.
We're here to assist

What Security Mistakes Put Custom EMR Systems at Risk?
Security issues in EMR systems usually come from practical gaps in access control, data protection, visibility, and late compliance decisions. These failures can lead to data exposure, audit issues, and operational disruption.

Weak authentication and access control
One of the most serious risks is giving users the wrong level of access or using weak authentication methods. Shared accounts, broad permissions, and poor role separation make it easier for unauthorized users to view or change sensitive data.
Insecure storage and transmission of health data
Health data must be protected both at rest and in transit. Common failures include weak encryption, insecure backups, and unsafe data exchange through APIs or third-party integrations. These gaps increase the risk of data leakage or interception.
Missing audit trails and monitoring
Without reliable audit logs and monitoring, organizations cannot clearly track who accessed data, what changed, or when suspicious activity happened. This makes incident response harder and weakens compliance readiness.
Delaying compliance and security planning until the late stages
Security and compliance should shape the system from the start. When they are treated as late-stage tasks, teams often add controls too late, which creates gaps, rework, and long-term risk. This is one of the most costly mistakes in custom EMR system development.
HIPAA-compliant app built with Medplum to support early cancer detection

How Do These Mistakes Affect EMR Project Outcomes?
Mistakes in EMR development do not stay isolated. They affect timelines, budgets, daily operations, and the ability of teams to rely on the system. Over time, these issues increase the overall cost of EMR and reduce the value the system is expected to deliver.
Cost overruns and delivery delays
Unclear scope, rework, and late changes increase both time and cost. As new requirements appear during development, teams adjust plans, extend timelines, and allocate more resources.
This leads to budget pressure and delayed releases. In many cases, organizations pay more for a system that still does not fully meet their needs.
Low adoption by clinicians and staff
When workflows are misaligned or the interface is hard to use, clinicians and staff avoid using the system where possible. They may rely on workarounds, duplicate tools, or incomplete documentation.
Low adoption reduces the effectiveness of the EMR and limits the return on investment. It can also affect care coordination and data quality.
Compliance exposure and legal risks
Gaps in security, auditability, and data handling increase the risk of non-compliance with healthcare regulations. Missing controls or incomplete records can create issues during audits or investigations.
This may result in penalties, legal exposure, and loss of trust from partners and patients.
Performance, reliability, and support issues
Weak architecture and rushed implementation often lead to slow performance, system instability, and frequent issues in production. As the system grows, these problems become harder to manage.
Support teams spend more time resolving incidents, and users face interruptions in their daily work. Over time, this affects both operational efficiency and confidence in the system.
How Can You Avoid the Top Mistakes in Custom EMR Development?
Avoiding common EMR issues comes down to early alignment, continuous validation, and planning for how the system will evolve. The focus should stay on real clinical use, because systems built on assumptions rather than current workflows tend to create more problems than they solve.
Involve healthcare stakeholders early
Strong EMR projects start with input from the people who will use and support the system. This includes clinicians, administrative staff, IT teams, and compliance specialists.
Early involvement helps define realistic requirements, uncover edge cases, and align expectations across teams. It also reduces the risk of misinterpretation during development and catches issues like incorrect field mapping before they become expensive to fix.
Prioritize security and compliance from day one
Security and compliance should shape system design, not follow it. Decisions around data access, storage, and auditability need to be built into architecture and workflows from the start. Inadequate testing at this stage is one of the most common reasons compliance gaps surface late, often after the system is already in use.
This approach reduces rework later and supports consistent handling of sensitive health data across the system, preventing it from becoming a siloed system that can't share information reliably with the rest of the care environment.
Build around workflows, not assumptions
Design decisions should be based on how care is delivered in practice. Mapping real workflows (including EMR templates that reflect how clinicians actually document care) helps ensure the system supports daily tasks without adding friction or contributing to longer patient visits.
Continuous validation with users during design and development keeps the product aligned with real-world usage.
Design for interoperability, continuous improvement, and future growth
An EMR system needs to connect with other platforms and adapt over time. Planning for integrations, data exchange standards, and modular architecture supports this from the beginning.
This is especially important when considering EHR vs. EMR scope, where systems may need to extend beyond internal workflows and support broader data exchange as requirements evolve.
Final Thoughts
Custom EMR projects tend to fail for predictable reasons. The risks, like unclear scope, weak workflow alignment, etc., build up over time and affect how the system performs in real clinical settings.
The impact is measurable. Healthcare continues to have the highest data breach costs, averaging $7.4 million per incident (IBM). At the same time, global IT spending is expected to exceed $6 trillion according to Gartner, which increases pressure to control the cost of EMR delivery and maintenance. High adoption rates, such as over 80% of providers using EHR systems, shift the focus from implementation to system quality and usability.
The value of a custom EMR depends on early decisions. Systems that align with workflows, support integrations, and meet compliance requirements from the start are easier to scale and maintain. Systems that do not often require ongoing fixes, which increases cost and reduces adoption.

Future outlook
Custom EMR systems are moving toward modular architectures, stronger interoperability, and tighter security controls. Standards like FHIR are becoming a baseline for data exchange, while AI-driven features are starting to support documentation and decision-making.
This increases both capability and complexity. Teams need to design systems that can evolve without major rework, while keeping data secure and workflows stable.
Our EHR|EMR development services

FAQ

The biggest mistakes in EMR system development include unclear project scope, ignoring real clinical workflows, weak UX design, poor architectural decisions, and underestimating integration complexity.
These issues often lead to rework, delays, and systems that do not support daily clinical tasks effectively. Security gaps and a lack of structured rollout also contribute to long-term problems with adoption and maintenance.
Custom EMR projects usually fail due to misalignment between the system and real-world healthcare operations. When requirements are not clearly defined, workflows are not validated, and users are not involved early, the final product does not match how teams work.
Poor workflow integration is one of the most common reasons systems struggle after launch, even when the underlying custom EHR development is technically sound. This leads to low adoption, decreased productivity, and ongoing fixes that stretch well beyond the go-live date.
Common security mistakes include weak access control, insecure data storage and transmission, missing audit logs, and late implementation of regulatory compliance requirements. Poor data migration practices also introduce risk. When patient records are transferred without proper data mapping, errors can surface in ways that are difficult to trace and costly to fix.
These gaps increase the risk of unauthorized access, data breaches, and audit failures. In healthcare, even small issues in data protection can have serious legal and operational consequences for patient care.
Poor workflows make EHR system development harder to get right and even harder to roll out successfully. Users may need to enter the same data multiple times, switch between disconnected screens, or follow steps that do not match the flow of care.
When standardized data formats are not applied consistently, it further compounds the problem. Systems struggle to share information cleanly, and staff lose confidence in what they see. This slows down work, increases errors, and reduces trust in the system. Without ongoing support and a clear plan for a successful EHR transition, teams often fall back on workarounds that undermine patient outcomes over time.

















 TechMagic Academy
TechMagic Academy